PBC Disease Stages
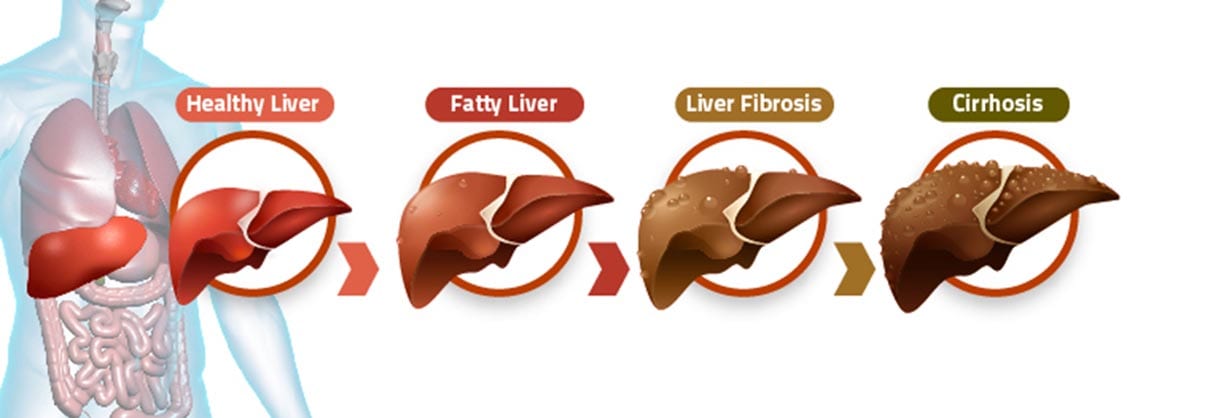
Although four (4) typical stages of evolution have been defined, the disease initially is focal with considerable overlap between stages in any one case.
First is inflammation of the medium-sized bile ducts and chronic inflammation of the portal tracts. Granulomas may be found. With progression of PBC, the portal tracts become distorted, inflammation spreads into the parenchyma, bile ducts proliferate intensely, and periportal fibrosis develops.
Progressive scarring continues with less bile duct proliferation and less inflammation. Fibrous bands link the portal tracts, and zone 1 cholestasis and Mallory hyaline can become evident. The end product is a firm, regular, intensely bile-stained cirrhosis, difficult to distinguish from other cirrhotic processes in the absence of granulomas and the pathognomonic bile duct lesions.
Stage 1: Portal Stage
Normal sized triads; portal inflammation, subtle bile duct damage. Granulomas – nodules filled with a variety of inflammatory cells – are often detected in this stage.
Stage 2: Periportal Stage
Enlarged triads; periportal fibrosis and/or inflammation. Typically characterized by the finding of a proliferation of small bile ducts.
Stage 3: Septal Stage
Active and/or passive fibrous septae.
Stage 4: Biliary Cirrhosis
Nodules present; garland or jigsaw pattern.
Although 4 typical stages of evolution have been defined, the disease initially is focal with considerable overlap between stages in any one case.
First is inflammation of the medium-sized bile ducts and chronic inflammation of the portal tracts. Granulomas may be found. With progression of PBC, the portal tracts become distorted, inflammation spreads into the parenchyma, bile ducts proliferate intensely, and periportal fibrosis develops.
Progressive scarring continues with less bile duct proliferation and less inflammation. Fibrous bands link the portal tracts, and zone 1 cholestasis and Mallory hyaline can become evident. The end product is a firm, regular, intensely bile-stained cirrhosis, difficult to distinguish from other cirrhotic processes in the absence of granulomas and the pathognomonic bile duct lesions.
Laboratory Findings
Early findings feature cholestasis with alkaline phosphatase elevated disproportionately greater than serum bilirubin and aminotransferases. In fact, the serum bilirubin is often normal early in the course of the disease. Serum bile acid concentration and gamma-glutamyl transpeptidase activity are elevated. Serum cholesterol concentration and total lipids usually are increased. Serum lipoproteins are increased, mainly because lipoprotein-X is present. Serum albumin is normal early in the course of the disease, but the globulins usually increase the serum IgM often to very high values. Antibodies against a component of the inner membrane of mitochondria (in 85% to 95% of patients) are important diagnostically, but they can also be found in some patients with HBsAg-negative chronic active hepatitis, making this differentiation difficult.
Prognosis
The course of PBC varies greatly. It may not diminish the quality or the duration of life. Of patients who present without symptoms, 50% show evidence of liver disease over the ensuing 15 yr. Slow progression suggests prolonged survival. A rising serum bilirubin, associated with autoimmune disorders, and advanced histologic changes indicate a poor prognosis.
PBC is one of the best indications for liver transplantation.
